Food-EPI
Select country tabs for individual Food-EPI reports
Effective government policies are essential to increase the healthiness of food environments and to reduce obesity, NCDs, and their related inequalities. Food environments are defined as the collective physical, economic, policy and socio-cultural surroundings, opportunities and conditions that influence people’s food and beverage choices and nutritional status. Unhealthy food environments lead to unhealthy diets and excess energy intake which have consequences in levels of morbidity and mortality. It is critical that Governments implement preventive policies and actions to match the magnitude of the burden that unhealthy diets are creating. Monitoring the level of implementation of the policies and actions recommended by the World Health Organization (WHO) is an important part of ensuring progress towards better nutritional health.
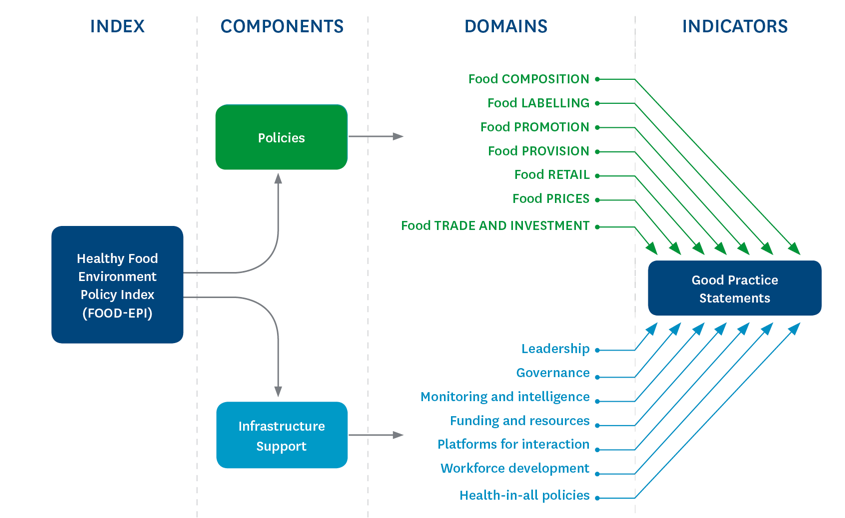
The Food-EPI index consists of two components (Policies and Infrastructure Support), 13 domains and 47 good practice indicators. A national expert panel aims to rate the level of implementation of policies on food environments by the Government against international best practice, and then, based on the implementation gaps, propose and prioritize key actions for implementation by the government.
The Healthy Food Environment Policy Index (Food-EPI)